 Staff work area (2) and toilet (3) are isolated from the patient care area (4). The anteroom (1) is an enclosed area with access from the outside. The gymnasium area is shown in Figure 1 as “large gymnasium” and encompasses 2,930 square feet, with a 10-foot ceiling, for a total air volume of 29,300 cubic feet.Īrchitectural drawing of the physical therapy gymnasium illustrating its conversion to negative-pressure isolation room. 
This area required several minor modifications to allow use of the equipment and to effectively isolate the air in the gymnasium from that of the rest of the hospital. The physical therapy gymnasium at our facility was used on April 28, 2003, to test the ability to create a negative air pressure environment in a large space not previously designed for such a use ( Figure 1 Our clinical engineering department performed all work in-house. Planning and work began approximately 6 weeks before the unannounced exercise was to be conducted. The personnel costs were estimated to be less than $2,000. 4 We assembled a team of mechanical engineers, safety personnel, physicians, industrial hygienists, and construction personnel to design, fabricate, and assemble the material required for the conversion. In designing the project's specification, we used the Centers for Disease Control and Prevention (CDC) Healthcare Infection Control Practices Advisory Committee Guidelines for Environmental Infection Control in Healthcare Facilities from 2003. This exercise was designed to assess whether the negative-pressure environment needed to isolate multiple patients can be achieved quickly and effectively using existing hospital space. This article describes a project designed to transform existing space within a hospital into an airborne infection isolation unit with the capacity to isolate large numbers of patients in a negative-pressure environment. Given the expense of either approach, we sought a means for mass isolation that would be inexpensive and feasible at most facilities. Such planning calls for airborne infection isolation that is well beyond the scope of current isolation practices at most hospitals and requires either retrofitting existing facilities or constructing new ones. 4 The risk of bioterrorism with a transmissible pathogen such as smallpox or plague has necessitated planning for the contingency of having to isolate large numbers of patients. Recent naturally occurring outbreaks of influenza or severe acute respiratory syndrome (SARS) have underscored the need to develop a flexible capacity for isolation to contain an outbreak. 
2 Negative-pressure rooms are generally expensive to build, with new construction costs, according to a 1988 figure, ranging from $40,000 to $50,000 per room. 
The use of personal respiratory protection is indicated for persons entering these rooms. The air in an airborne infection isolation room is preferably exhausted to the outside, but may be recirculated, provided that the return air is filtered through a high- efficiency particulate air (HEPA) filter. This isolation area receives 6 to 12 air changes per hour and is under negative pressure so that the direction of airflow is from the outside adjacent space (eg, corridor) into the room. 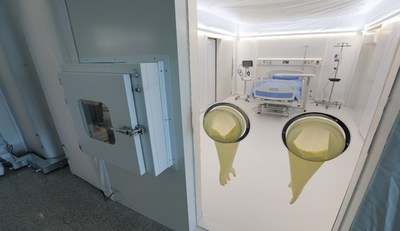
1Īirborne infection isolation refers to the isolation of patients infected with organisms spread by airborne droplet nuclei less than 5 μm in diameter. Isolation has been effectively accomplished using a single patient room with negative air pressure and a ventilation system separated from the rest of the hospital. Patients with communicable diseases, such as influenza and tuberculosis, often require respiratory isolation precautions to reduce the chance of transmission. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
